OVERVIEW
This piece explored how persistent challenges in benefits management impact cost and operational efficiency. It also defines how Third Party Administrators (TPAs) leveraging AI-driven automation are modernizing enrollment, plan administration, and compliance as essentials for better performance guarantee.
Padmanabha “PSB” Bhatta | December 13, 2025
How Benefit Management is Evolving for TPAs?
The U.S. healthcare TPA market is huge, valued at over $100 billion in 2024, projected to reach $129 billion by 2030, and growing at a CAGR of 3.9%1. Research from the Kaiser Family Foundation also showed a significant 65% of covered employees in the US are enrolled in self-funded plans, with 83% of them employed at large organizations.2
As the administrative backbone for self-funded companies, TPAs are crucial in benefits management as they optimize plan funds, reduce administrative burdens, and improve members engagement through tailored programs.3
In the race to capture self-funded groups at scale, adopting AI and automation is the new alpha for speed to market while effectively improving performance guarantees.
Tech Snippet
How does AI and automation enhance benefits management for TPAs?

AI agents and advanced language models help analyze and score onboarding data to flag priority cases for review, personalize member communications, and automate contracting—making the benefits process and decision-making smoother and smarter.
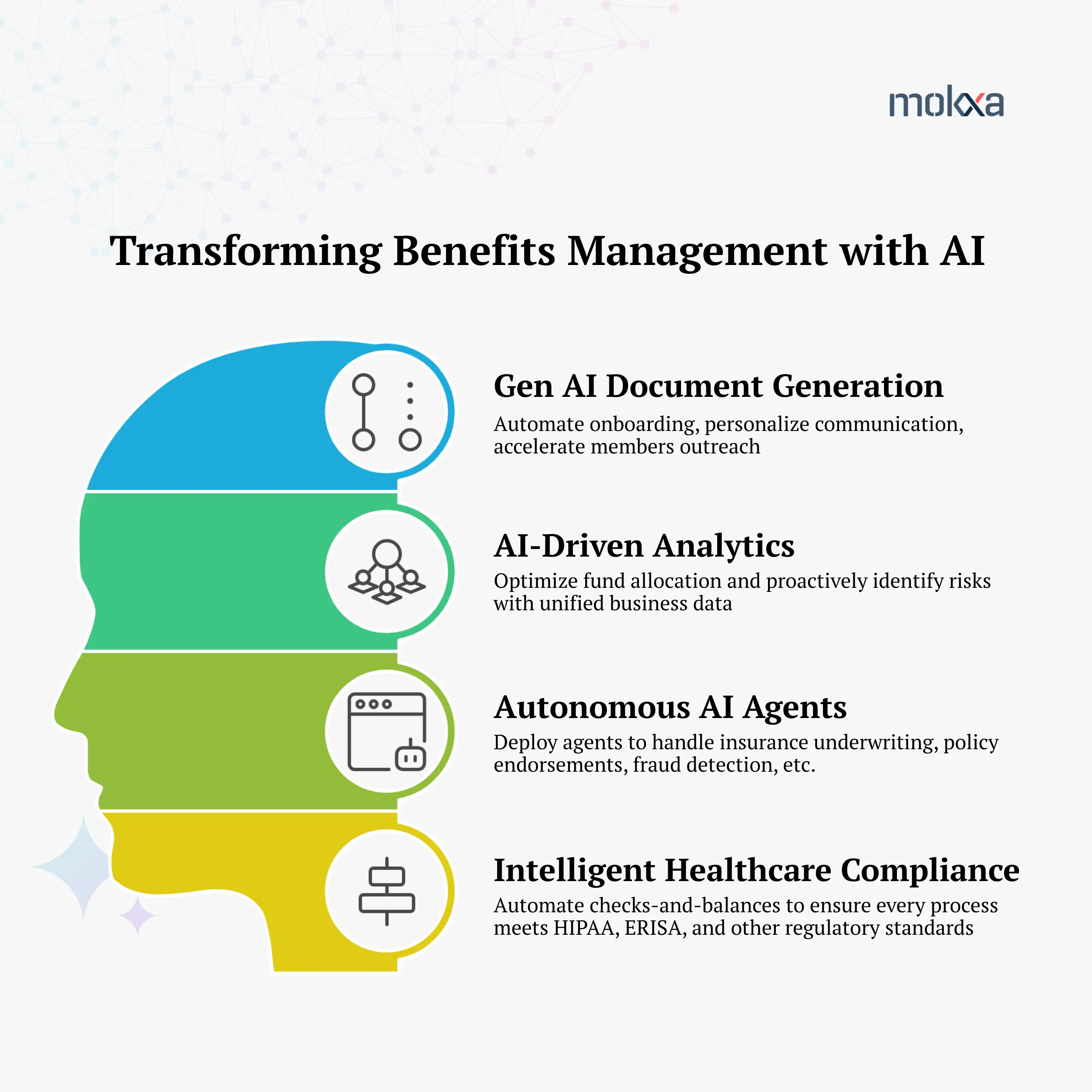
Key strategies for improving benefits management performance
Accenture’s research shows AI adoption in benefits management delivers sizable operational cost savings, faster turnaround, and better member health outcomes4. From enrollment and onboarding to plan administration and compliance, benefits administration is evolving quickly thanks to AI.
Generative AI automates document generation with personalized member outreach, boosting engagement by 20%5. Capabilities of AI-driven analytics when integrated with clinical, financial, and utilization data in real-time, will optimize fund allocation and identify risks early.
Agentic AI learns, adapts, and makes independent decisions to deliver dynamic, context-aware solutions. It dramatically improves onboarding, insurance underwriting, policy endorsement, renewal & cancellation, and reporting, moving enrollment from a ’48-hour’ review cycle to an instant automation stream.
These wins enable TPAs to effectively customize and manage their plan portfolios, while aligning compliance with HIPAA, ERISA, and other federal/state regulations.
Biz Snippet
Why is AI-powered benefits management vital for TPA performance guarantees?

It reduces costs, enhances compliance reliability, speeds up service delivery, and personalizes member engagement—key levers for consistent contract performance and customer trust.
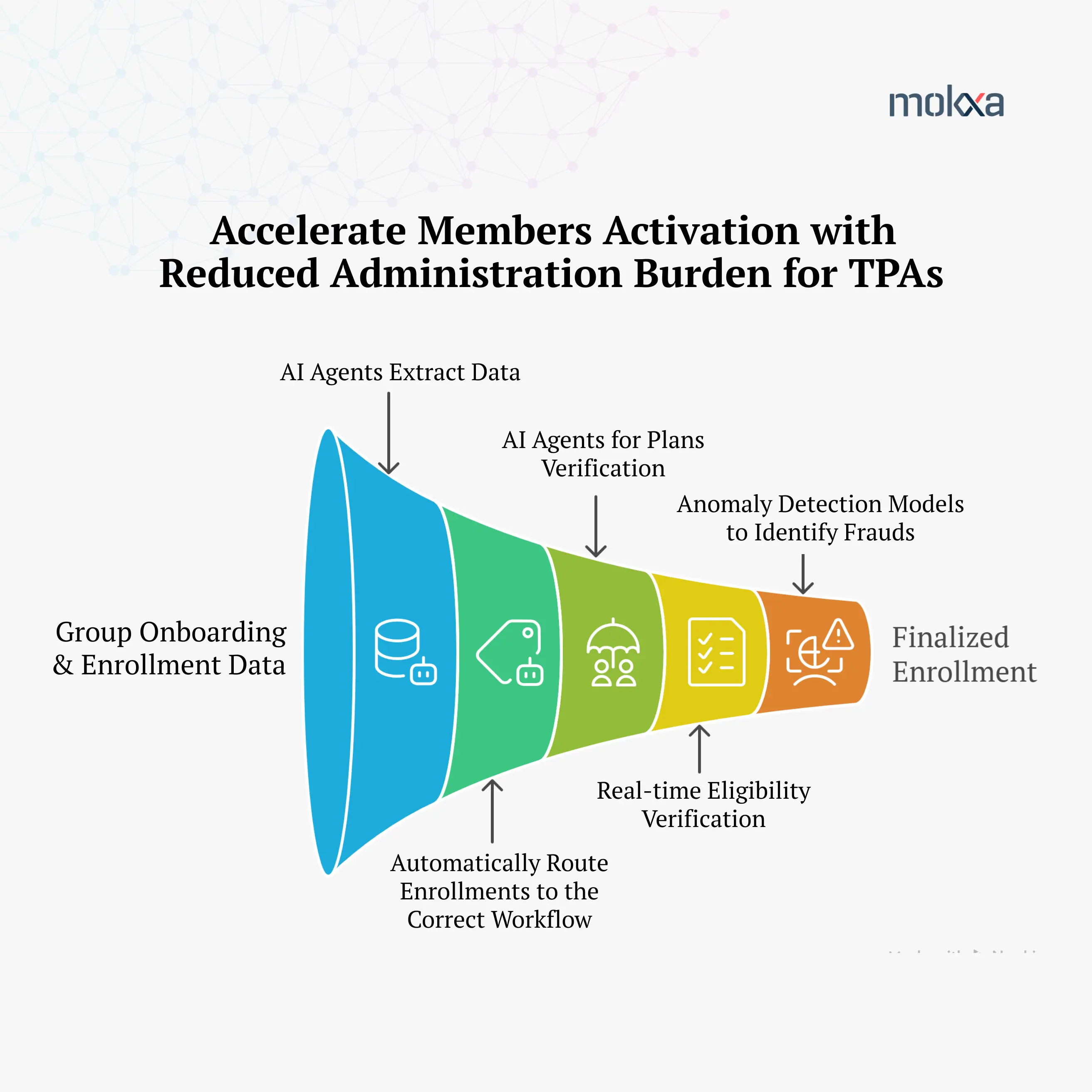
Building an AI-ready Benefits Management Capacity
To deliver faster speed-to-value amid rising regulations, costs, and member expectations, TPAs must move from reactive workflows to proactive AI-enabled benefits management.
- Introduce AI Agents that can extract, ingest, and classify all incoming enrollment data, whether submitted via paper forms, portals, or electronic feeds.
- Automatically route enrollment types—from Medicare Advantage groups to self-insured plans—to the correct onboarding workflows for parallel processing.
- Reduce group onboarding from weeks to days. Agentic AI can accelerate plans configuration, tiered networks, cost-sharing arrangements and regulatory compliance.
- Cross-reference member enrollment data against their eligibility in real-time. Flag inconsistencies or missing information for rapid resolution.
- Use advanced pattern recognition and anomaly detection models to identify potential fraud or data entry errors before member eligibility is finalized in the benefits system.
The result is a transparent, precise benefits management process that accelerates member activation, reduces administrative burden, and strengthens client confidence.
Expert Speak
We've seen large TPAs deconstruct legacy benefits management processes to build AI capacity for

enterprise automation without ripping the core. This non-disruptive, scalable process orchestration is the fastest, secured way to unlock new capabilities and enhance performance guarantee in healthcare.
Padmanabha “PSB” Bhatta
Chief Customer Success Officer
TPA Mandates for Seizing the $129B Market Opportunities with AI-led Enterprise Transformation
- The growing U.S. TPA market (projected $129B by 2030) demands improved benefits management to control costs and enhance member engagement.
- AI adoption delivers cost savings, faster onboarding, enhanced compliance, and personalized experiences, enabling TPAs to meet performance guarantees.
- Agentic and Generative AI automate enrollment with compliance, cutting onboarding times up to 50% and improving accuracy and transparency.
- Extend legacy systems and scale up with Agentic AI application fabric to proactively manage funds, identify risks early, and make better business decisions.
- Shifting to AI-led solution orchestration will transform benefits administration from reactive to proactive for scalable operations and better client trust.
Scalable Workflow Automation, Delivering 50% Productivity Growth and ROI Gains
Go to Case Study
Sources
- Next Move Strategy Consulting: The U.S. Health Insurance TPA Market Size Analysis by 2030
- Kaiser Family Foundation: 2023 Employer Health Benefits Survey | KFF
- Personify Health: Optimizing Health Plans Using a Third-Party Administrator (TPA)
- Accenture: Humanising Healthcare Payer with Technology
- McKinsey: Insurance 2030—The impact of AI on the future of insurance


